
I have ENDOMETRIOSIS or suspect ENDOMETRIOSIS, but I do not want a pregnancy.
Treatment of pain due to ENDOMETRIOSIS
ENDOMETRIOSIS is a chronic disease. In that sense, there is no cure for ENDOMETRIOSIS, but the symptoms can be reduced with the right treatment. Women with ENDOMETRIOSIS have either pain, fertility problems or they have both.

Can I take analgesics (painkillers) for pain due to ENDOMETRIOSIS?
Analgesics, like non-steroidal anti-inflammatory drugs (NSAIDs), are medical therapies that influence how the body experiences pain. These therapies are not specific for endometriosis-associated pain, and they do not alter any disease mechanism in the body like the hormone treatments do.
Analgesics have little side-effects, they are cheap, easily accessible, and widely used, but very little studies have investigated whether they actually help in reducing endometriosis-associated pain. Long-term use of NSAIDs can be associated with side-effects, such as stomach problems. Therefore, considering protection of the stomach is advisable.
Pain medication NSAIDs or other analgesics (either alone or in combination with other treatments) can be used to reduce endometriosis-associated pain.
Endometriosis is a chronic disease. In that sense, there is no cure for endometriosis, but the symptoms can be reduced with the right treatment. Women with endometriosis have either pain, fertility problems or they have both.
What are the options for hormonal treatment of pain?
Hormonal treatments in clinical use are:
- Hormonal contraceptives (cyclical use or continuously).
- Progestogens, including intra-uterine devices.
- GnRH agonists.
- GnRH antagonists.
- Aromatase inhibitors. While effective for treating endometriosis.
Hormone treatments may also induce side-effects such as headaches, acne, weight gain, vaginal spotting, fatigue, and hot flushes. Effects differ strongly between treatments and between patients.

How does hormone treatment work?
Endometriosis is a problem associated with a woman’s menstrual cycle and dependent on the activity of estrogens. One aim of hormone treatment for pain in women with endometriosis is lowering the estrogen level. Another aim is to reduce the effect of estrogen on the endometriotic tissue. It is important to know that hormone treatment probably does not cure endometriosis. Hormone treatment suppresses the activity of the disease and hence the pain symptoms.
However, after discontinuation of the treatment symptoms tend to recur. It is not known which patients will have a relapse of pain symptoms.
Combined hormonal contraceptives are widely used for contraception and generally accepted as treatment for endometriosis-associated symptoms. They contain low doses of hormones (estrogen and progesterone) and can reduce pain associated with endometriosis by stopping follicular growth and hence reducing the production and concentration of estrogens.
Low estrogens stop the activity of the growth of the endometrium in and outside the uterus, and thus pause endometriosis. The progesterone in the pill decreases the activity of the endometrium and the endometriotic tissue directly. The side effects are limited, and hormone contraceptives are not expensive. There are different options for hormonal contraceptives: the oral contraceptive pill (taken with or without a monthly pill-free week), a vaginal contraceptive ring, or a transdermal patch.
Progestagens , which are substances very similar to the body’s progesterone, can be used in different forms: orally, as a 3-monthly injection, a levonorgestrel-releasing intrauterine system, or a contraceptive implant under your skin. Different types of progestagens are medroxyprogesterone acetate (MPA), dienogest, or cyproterone acetate. Progestogens are also used as contraceptives, either in combination with estrogen or by themselves (‘minipill’). Progestogens are relatively inexpensive. The different types of progestagens have different side effects.
A levonorgestrel-releasing intrauterine system is a small device that is inserted in the uterus and releases low levels of progesterone. It is frequently used for contraception; it has limited side effects and is user-friendly. In women with endometriosis, it is an option for reducing symptoms of pain.
A contraceptive implant which is inserted under your skin, usually in your arm, can also stop your periods and may help with endometriosis-associated pain symptoms.
GnRH agonists induce a very low estrogen level by stopping the follicular growth in the ovary completely. GnRH agonists can be taken intranasally, or through subcutaneous injection as a depot working either one or three months. Some of the most common GnRH agonists are nafarelin, leuprolide, buserelin, goserelin and triptorelin. GnRH agonists have more side effects than oral contraceptives and progestagens and are more expensive.
The side effects of GnRH agonists are related to the low level of estrogens and are comparable to the consequences of the menopausal status. These so-called hypo-estrogenic symptoms are hot flushes and night sweats, vaginal dryness and related pain during intercourse, and influences on the mental health up to depressive feelings. In the long-term GnRH agonists are associated with osteoporosis. To reduce these symptoms, clinicians are recommended to prescribe hormone add-back therapy as soon as GnRH agonists are started. Some doctors may start add-back therapy a few weeks or months into your GnRH agonist treatment. Hormone add back means adding a combination of estrogens and progesterone (oral contraceptives).
This add back therapy takes away the side effects while the therapeutic effect is maintained. Since adolescents and young women have not reached their optimal bone density, it is advisable not to use GnRH agonists/ GnRH antagonists in these women unless as second line treatment and if other treatments with less severe side effects have not helped or are not tolerated.
Aromatase inhibitors stop an enzyme (aromatase) that is needed in the production of estrogens in several cells of the body. The result is a very low estrogen level. These drugs have been used in other diseases, but they are not well studied yet in endometriosis. Due to the side effects (vaginal dryness, hot flushes, diminished bone mineral density), aromatase inhibitors should only be prescribed to women in severe pain after trying all other options of medical and surgical treatment.
Is surgical treatment an option for relieving pain symptoms?
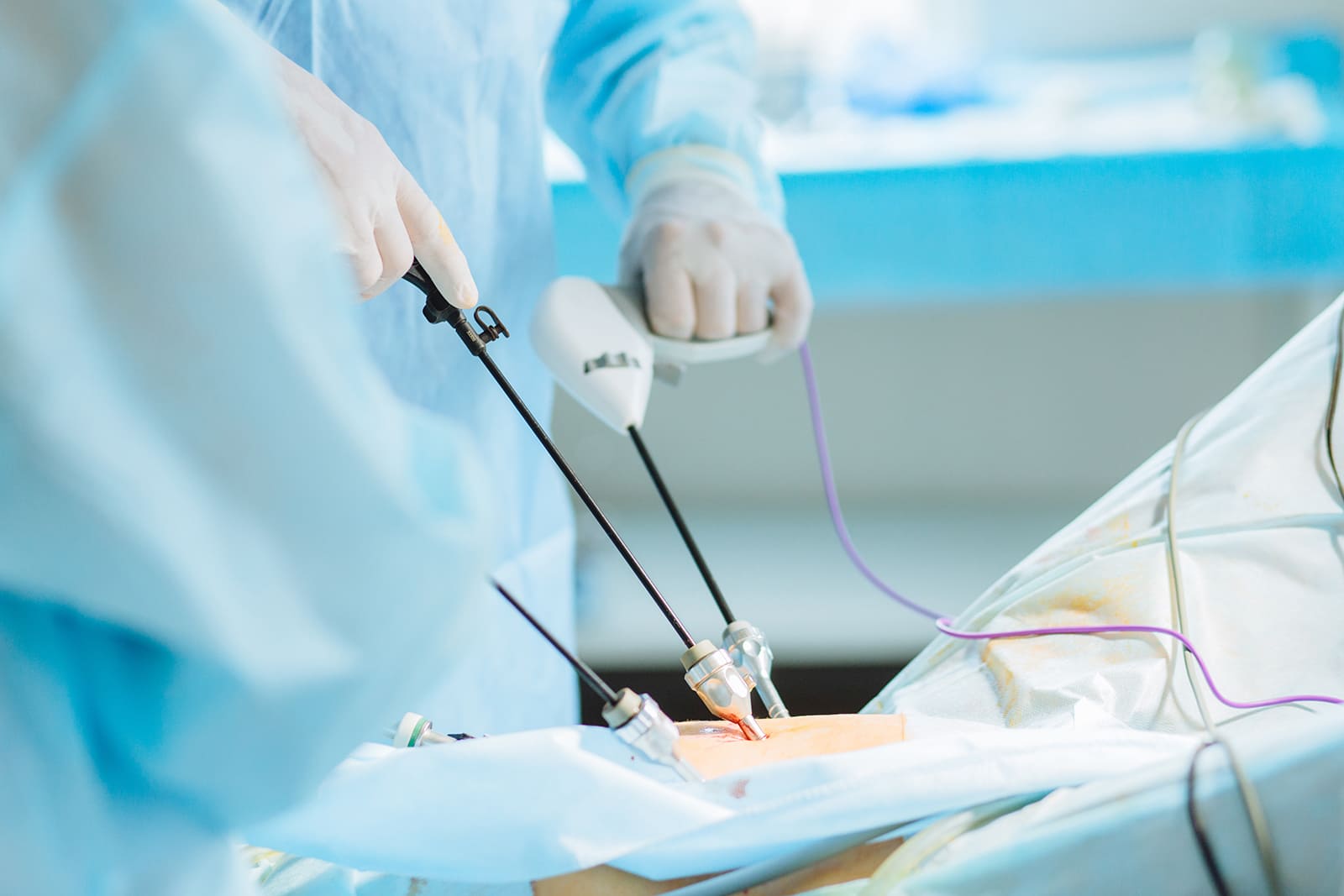
Surgical treatment of endometriosis focuses on the elimination of peritoneal endometriosis/ endometrioma/deep endometriosis and division of adhesions. In the past, open surgery (laparotomy) was used routinely. Nowadays, keyhole surgery (laparoscopy) is used frequently and preferred since it usually results in less pain, shorter hospital stay, quicker recovery and a smaller scar.
Clinicians should consider surgical treatment (elimination of endometriotic lesions) when they see endometriotic lesions during laparoscopy for diagnosis. Surgical treatment should be considered as one of the options to reduce endometriosisassociated pain.
You may be offered hormone treatment after surgery, as it could improve the immediate outcome of surgery for pain and could prevent recurrence of disease/symptoms. When you desire pregnancy shortly after surgery, hormone treatment should be avoided. While surgery is generally effective for relieving pain symptoms, it may not always improve all symptoms and relieve symptoms only partially or temporarily.
Hysterectomy If you have completed your family and other treatments have not worked, you may consider, removal of the uterus (hysterectomy) with or without removal of the ovaries. This is a radical and irreversible option which results in so called surgical menopause and menopausal symptoms (hot flushes, etc) if the ovaries are removed at the same time.
You should know that hysterectomy does not always solve the problem, since sometimes endometriosis inadvertedly is left behind and hence the pain symptoms remain present. Hysterectomy may help if your symptoms are mostly due to adenomyosis and should be considered if other treatments have failed.
Hysterectomy can be performed if you failed to respond to more conservative treatments and if you no longer wish to conceive. Still, you should be aware that hysterectomy will not necessarily cure the symptoms or the disease.
The treatment of choice for pain related to endometriosis outside the pelvis (extrapelvic endometriosis) largely depends on the location of the endometriosis.
- For abdominal extrapelvic endometriosis: Surgical removal is the preferred treatment, when possible, to relieve symptoms.
- Hormone treatment may also be an option when surgery is not possible or acceptable.
- For thoracic endometriosis (in the chest), Hormone treatment can be offered. If surgery is indicated, it should be performed involving a thoracic surgeon and/or other relevant specialists.
